Chapter 14 – Musculoskeletal
Hip Fracture – Femoral Neck Fracture
ACR – MSK – Acute Hip Pain – Suspected Fracture
Case
Femur fracture
Clinical:
History – This 88 year old male fell at the Nursing Home and had right hip pain.
Symptoms – The hip was painful and the patient couldn’t weight bear.
Physical – The right leg was shorter than the left and the right foot was turned in a lateral direction. The leg pulses were normal. Range of motion of the left hip was limited by severe pain.
DDx:
Hip fracture
Hip dislocation
Femur fracture
Pelvic fracture
Imaging Recommendation
ACR – MSK – Acute Hip Pain – Suspected Fracture, Variant 1
X-Rays
Imaging Assessment
Findings:
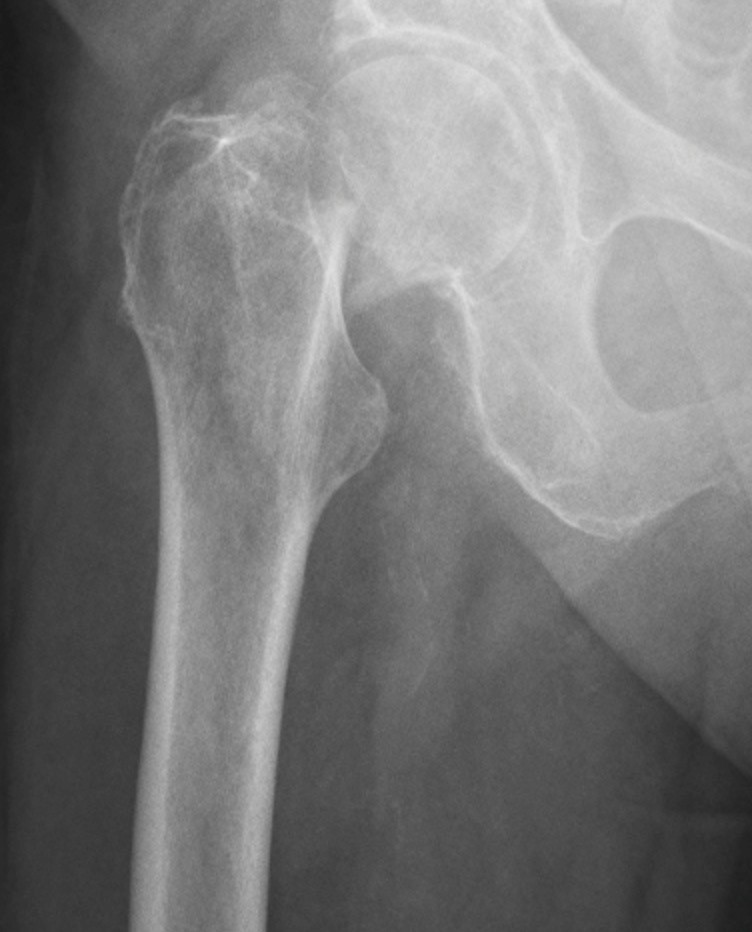
There was a fracture of the high femoral neck on the right. This fracture was impacted. The distal femur was displaced cranially and laterally.
Interpretation:
Femoral Neck fracture.
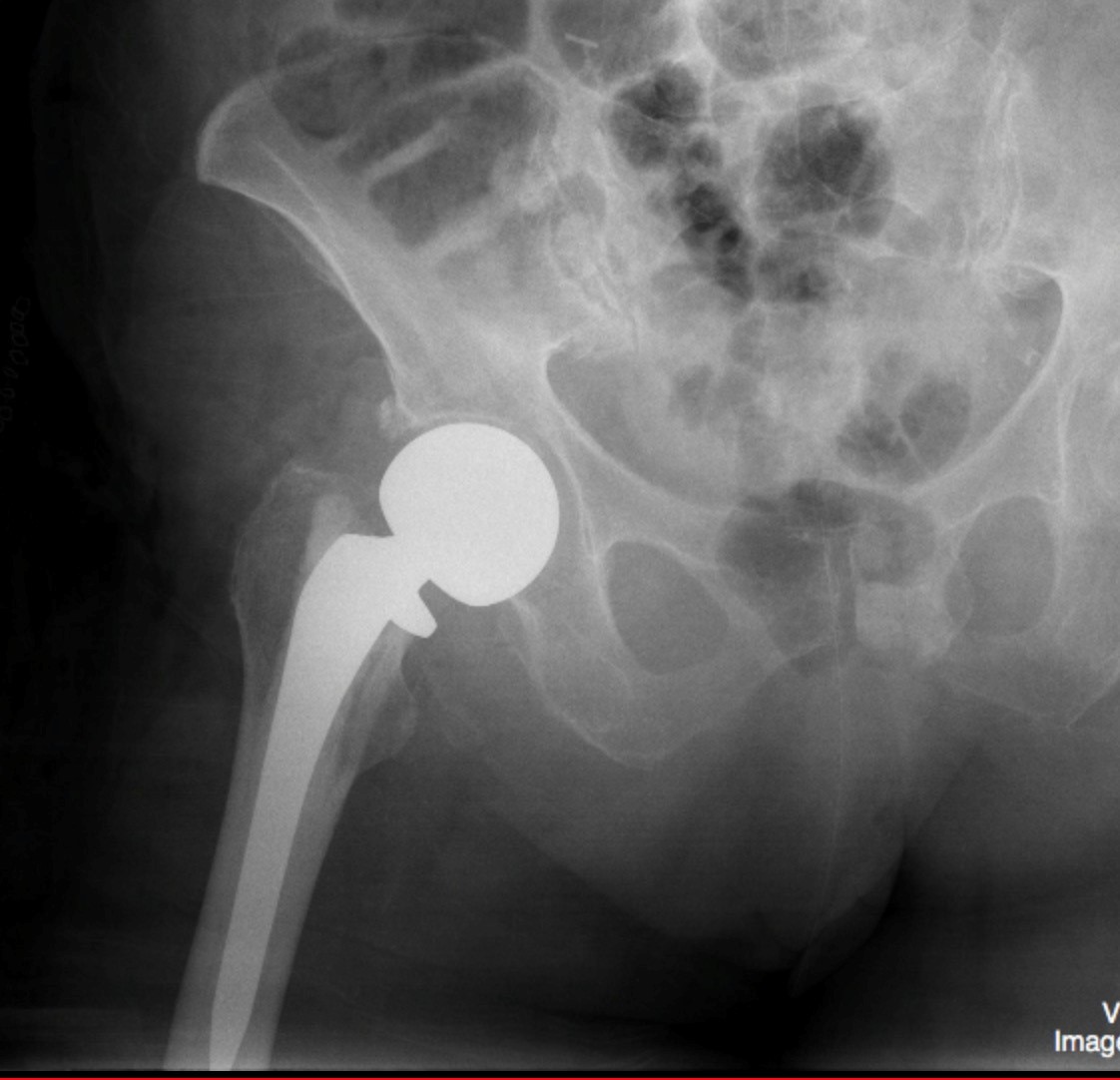
Subsequent images revealed that the patient had surgical management of this fracture resulting in the placement of an Austin-Moore prosthesis.
Diagnosis:
Femur fracture
Discussion:
Femoral neck fractures are a subset of proximal femoral fractures. The femoral neck is the weakest part of the femur. Since disruption of blood supply to the femoral head causes significant morbidity, diagnosis and classification of these fractures is important. Avascularity of the femoral head is more common with fractures that are cranially situated in the femoral neck. Neck of femur fractures are considered intracapsular fractures.
Intracapsular fractures include:
- Subcapital: femoral head/neck junction
- Transcervical: mid-portion of femoral neck
- Basicervical: base of femoral neck
Mechanism:
- Falls in the elderly;
- Trauma (e.g. motor vehicle collisions) in younger patients.
In elderly patients, the mechanism of injury varies from falls directly onto the hip to a twisting mechanism in which the patient’s foot is planted and the body rotates. The mechanism in young patients is predominantly axial loading during high energy trauma, with an abducted femur position resulting in a femoral neck fracture while an adducted femur position often results in a fracture-dislocation of the hip with secondary acetabular injury.
X-ray findings may include:
- Shenton’s line disruption: loss of contour between normally continuous line from medial edge of femoral neck and inferior edge of the superior pubic ramus
- Lesser trochanter is more prominent due to external rotation of femur
- Femur often positioned in flexion and external rotation (due to unopposed iliopsoas)
- Asymmetry of lateral femoral neck/head
- Sclerosis in fracture plane
- Smudgy sclerosis from impaction
- Bone trabeculae angulated
- Non-displaced fractures may be subtle on x-ray
Treatment:
Significant complications such as avascular necrosis (AVN) and non-union are very common without surgical intervention. The treatment options include non-operative management, internal fixation or prosthetic replacement.
Internal fixation can be performed with multiple pins, intramedullary hip screw (IMHS), crossed screw-nails or compression with a dynamic screw and plate.
Replacing the femoral head is achieved with either hemiarthroplasty or total hip arthroplasty.
Prognosis is varied, but is complicated by advanced age, as hip fractures increase the risk of death and major morbidity in the elderly. High morbidity and mortality associated with hip and pelvic fractures after trauma has been well documented.
The risk of AVN depends on the fracture. The Delbet classification correlates with the risk of AVN:
| Type | Description | Risk of AVN |
| Type 1 | Transphyseal | ~ 90% |
| Type 2 | Subcapital | ~ 50% |
| Type 3 | Basicervical / transcervical | ~ 25% |
| Type 4 | Intertrochanteric | ~ 10% |
Table 14.3 Delbet Classification for risk of AVN with femoral neck fracture. https://radiopaedia.org/articles/femoral-neck-fracture
As a general rule, internal fixation is recommended for young, otherwise fit patient with small risk for AVN. While prosthetic replacement is reserved for fractures with high risk of AVN and the elderly.
Attributions
Figure 14.12A X-ray of the femur, pre-operative femoral neck fracture by Dr. Brent Burbridge MD, FRCPC, University Medical Imaging Consultants, College of Medicine, University of Saskatchewan is used under a CC-BY-NC-SA 4.0 license.
Figure 14.12B X-ray of the femur, post-operative arthroplasty by Dr. Brent Burbridge MD, FRCPC, University Medical Imaging Consultants, College of Medicine, University of Saskatchewan is used under a CC-BY-NC-SA 4.0 license.

